Where greater detail inspires greater confidence
We offer comperehensive prenatal imaging services as well prenatal screening and tests with expert radiologists, sonographers, and genetic counsellors.
Our pregnancy scans allow us to examine your growing baby to check fetal growth, make sure that anatomical development is normal for each gestational period, and confirm fetal wellbeing. They are typically performed during each trimester of your pregnancy.
Although you may get other scans or reviews if your doctor requests them.
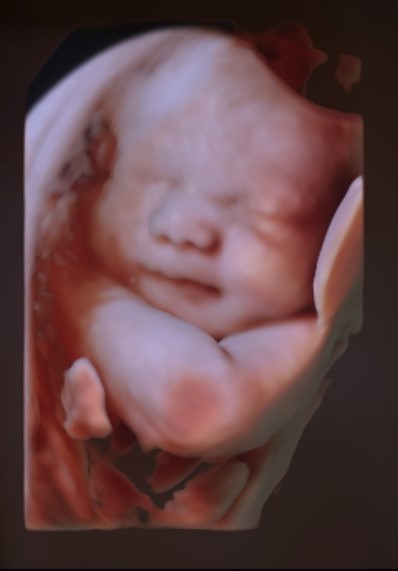
These detailed scans include 2D (black and white), 3D (coloured) and 4D (video loops), enabling us to identify many significant anomalies. Your scan will be discussed with you on the day, and you will receive the scan report as well as printed and digital copies of your pictures to take with you.
Early dating and viability scans are performed to
Each ultrasound examination is a snapshot in time of your pregnancy, and in the first six weeks, ultrasound may be nonspecific and require correlation with either an additional follow up scan and/or a repeat blood test of your hCG hormone level.
NIPT is the most accurate screening test for Down syndrome. It also screens for other chromosome conditions, trisomy 13 and trisomy 18. There are also options to screen for rarer chromosomal conditions and to find out the sex of the baby.
As the NIPT is a screening test, the results for the health conditions come back as either low probability or high probability for each condition. The NIPT is over 99% accurate for fetal sex. NIPT is a blood test that can be done from 10+3 weeks in pregnancy. The results usually take about a calendar week (approximately 5 working days). There is currently no medicare rebate for NIPT.
At SO+GI Scan, there are different ways that NIPT is arranged:
Everyone who has NIPT at SO+GI Scan will have a consultation with the genetic counsellor before the test to discuss the best options for them, and results will be called out with post-test counselling if required.
An ultrasound scan between 11+1 and 13+6 weeks can screen for chromosomal concerns and for structural anomalies. Ideally at SO+GI Scan these ultrasounds are booked between 12+3 and 13+6 weeks.
This scan looks at the baby in detail and is an early anatomy scan which can identify some major structural anomalies.
Combined first trimester screening (CFTS) involves information from this scan and a blood test for free βhCG and PAPP-A done at least 3 days prior to the scan. These results are used to calculate the chance the baby has a chromosome condition, including Down syndrome (trisomy 21), trisomy 13 or trisomy 18. If you have already had a low probability NIPT result we do not need to do this calculation as the NIPT is more accurate.
Preeclampsia occurs in about 3% of pregnancies (1 in 33) and can cause high blood pressure. In some severe cases it can cause organ damage for mothers, affect fetal growth and cause early delivery. Starting aspirin before 16 weeks can prevent or delay the onset of preeclampsia for many women.
The preeclampsia screen is done with the NT scan at 12 – 14 weeks, when the preeclampsia screen has been requested by your doctor, and involves:
The risk assessment can be done without the blood test, but it is less accurate – so less women end up in the low chance group.
The morphology scan is performed between 19 and 21 weeks. This scan examines the structure of the baby as well as checking on the placental position, how much amniotic fluid there is and the cervix length.
We use this scan to review the fetal structures in detail. At this stage we are able to detect many structural concerns, but not all. Some possible anomalies are still too small, some may develop later, and some can’t be seen on ultrasound.
Sometimes the baby is in a position that makes it hard to see, or for some other technical reason we don’t get all the measurements or see all the details we expect to see on this scan. We may ask you to go for a walk or have a cold drink to allow the baby to move into a better position and sometimes we will arrange for you to come back another day to finish the scan.
Some people are referred for a scan or scans after the morphology scan into the third trimester for a number of reasons.
These scans are used to:
We can estimate fetal weight based on the scan, but it can vary quite a lot at birth. We may also be able to get detailed 3D pictures of your baby’s face, depending on their position.
Invasive testing are procedures during pregnancy which offer diagnostic testing of the baby for chromosomal conditions such as Down syndrome, or single gene conditions such as cystic fibrosis. Invasive testing may be discussed with or offered to patients for a variety of reasons, most commonly those who have had a high-risk result on screening tests such as combined first trimester screening, NIPT or carrier screening, for family history, or after an anomaly is seen on an ultrasound.
There are two different options available for invasive testing, chorionic villus sampling and amniocentesis.
CVS can be done after 11 weeks and involves inserting a fine needle through the mother’s abdomen under ultrasound guidance to get a sample from the placenta. There is a small risk of miscarriage, up to 1 in 100. While the results are usually clear, occasionally they may be difficult to interpret and an amniocentesis may also be required.
An amniocentesis can be done after 16 weeks and involves inserting a fine needle through the mother’s abdomen under ultrasound guidance in order to get a sample of the amniotic fluid from around the baby, which contains cells from the baby. There is a small risk of miscarriage, up to 1 in 200.
If the testing is for chromosomal concerns, generally there will be an interim result available in 1-2 working days, and a final result in 5-10 working days. The time- frame for single gene testing results vary depending on the gene and testing laboratory.
You can speak to the genetic counsellor regarding whether you require invasive testing, which test is best for you and your situation, and what they involve in more detail.







